Rheumatology
There is something quietly devastating about waking up every morning with joints that feel like they have aged forty years overnight. For millions of patients across the UAE and beyond, that is not a metaphor — it is Tuesday. Rheumatology sits at the intersection of immunology, musculoskeletal medicine, and systemic disease management, and yet it remains one of the most underappreciated specialities in modern clinical practice. If you work in healthcare, understanding rheumatology deeply is no longer optional — it is essential.
What Rheumatology Actually Covers
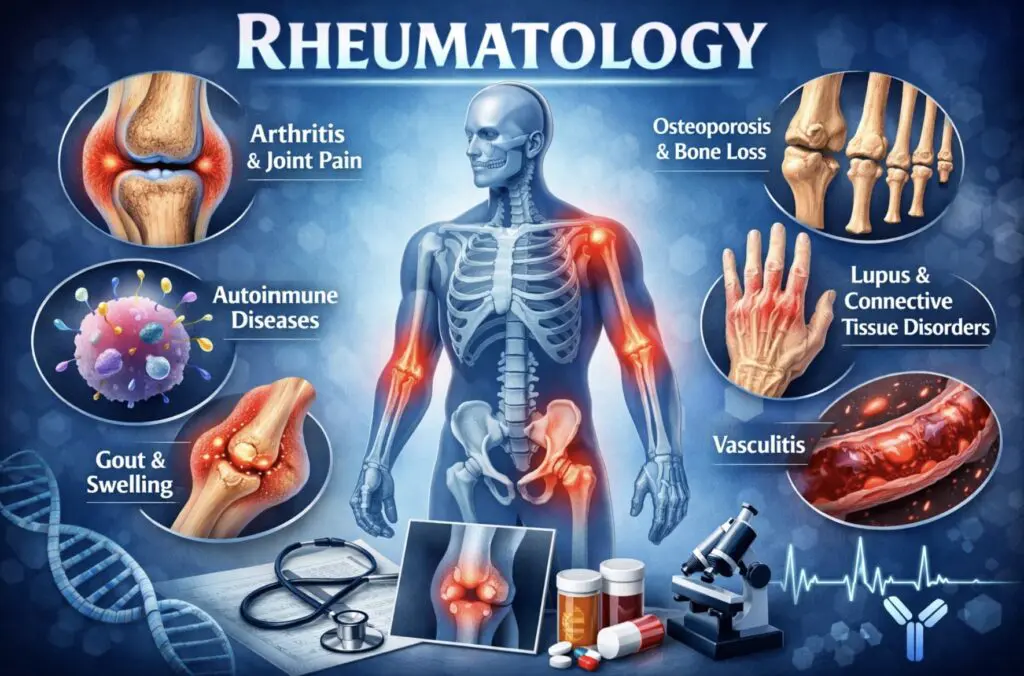
Rheumatology is the branch of internal medicine that focuses on diagnosing and treating musculoskeletal disorders, systemic autoimmune conditions, and inflammatory diseases. The scope extends well beyond joints. Rheumatologists routinely manage conditions including rheumatoid arthritis (RA), systemic lupus erythematosus (SLE), ankylosing spondylitis, psoriatic arthritis, gout, vasculitis, Sjögren’s syndrome, and systemic sclerosis. A common misconception, even among general practitioners, is that rheumatology only concerns older adults. Juvenile idiopathic arthritis (JIA), lupus, and reactive arthritis frequently present in younger populations. Early referral, therefore, plays a decisive role in long-term joint preservation and quality of life outcomes.
The Immunological Underpinning of Rheumatic Diseases
At the core of most rheumatic diseases lies dysregulation of the immune system. In conditions such as rheumatoid arthritis, the body’s adaptive immune response — particularly T helper cells and B lymphocytes — mistakenly targets synovial tissue. This chronic synovitis drives cartilage degradation and bony erosions over time. Pro-inflammatory cytokines, especially TNF-alpha, IL-6, and IL-17, orchestrate much of this damage.
Understanding these cytokine pathways has completely transformed treatment paradigms over the past two decades. The introduction of biologic disease-modifying antirheumatic drugs (bDMARDs) — including TNF inhibitors such as adalimumab and etanercept — marked a watershed moment in rheumatology. More recently, Janus kinase (JAK) inhibitors like baricitinib and upadacitinib have offered oral therapeutic options with targeted intracellular signalling blockade. Clinicians selecting between conventional synthetic DMARDs (csDMARDs), biologics, and JAK inhibitors must weigh comorbidities, infection risk, cardiovascular profile, and patient preference carefully.
Diagnosing Rheumatic Conditions: The Clinical Challenge
Rheumatology diagnosis rarely follows a straight line. Seronegative arthropathies, in particular, can evade detection for months or years. A patient presenting with inflammatory back pain, enthesitis, and dactylitis may satisfy the ASAS criteria for axial spondyloarthropathy long before MRI sacroiliac joint changes become radiographically evident. Clinicians must rely on a synthesis of clinical history, physical examination, laboratory biomarkers (anti-CCP antibodies, ANA titres, complement levels, and inflammatory markers), and imaging.
Point-of-care musculoskeletal ultrasound has grown significantly in rheumatology practice, allowing real-time assessment of synovitis, tenosynovitis, and erosive change at the bedside. Power Doppler imaging further distinguishes active inflammatory disease from structural damage — a distinction that directly informs treatment escalation decisions.
Treat-to-Target: The Modern Standard of Care
The treat-to-target (T2T) strategy has redefined how rheumatologists approach disease management. Rather than aiming broadly for symptom relief, T2T mandates the pursuit of clinical remission or low disease activity as a measurable endpoint, reassessed at regular intervals using validated composite scores such as the DAS28, SDAI, or CDAI. This approach has dramatically improved functional outcomes and reduced structural joint damage in RA and psoriatic arthritis alike.
For patients attending a rheumatology hospital in Dubai, this treat-to-target framework has become increasingly standard, reflecting the global shift towards precision medicine in rheumatology. International centres now routinely integrate shared decision-making into these protocols, ensuring patients understand their treatment goals and remain active participants in managing their condition.
The Multidisciplinary Dimension of Rheumatology Care
Rheumatic diseases rarely remain confined to joints. Systemic lupus erythematosus can involve the kidneys, central nervous system, haematological system, and pericardium simultaneously. Systemic sclerosis carries significant pulmonary and gastrointestinal complications. Rheumatoid arthritis increases cardiovascular risk substantially — a fact that must inform screening and pharmacotherapy choices.
This systemic complexity means that effective rheumatology care demands genuine multidisciplinary collaboration. Nephrologists, cardiologists, pulmonologists, dermatologists, and ophthalmologists regularly co-manage patients alongside rheumatology teams. Allied health professionals — physiotherapists, occupational therapists, specialist rheumatology nurses — play an equally critical role in functional rehabilitation and patient education.
Emerging Therapeutics and the Future of Rheumatology
The pipeline for rheumatology therapeutics continues to grow. B-cell-targeted therapies, IL-23 inhibitors, complement pathway modulators, and cell-based therapies are all under investigation for conditions ranging from lupus nephritis to systemic vasculitis. Biosimilar medications have broadened access to biologic therapy considerably, an important development given the cost burden that advanced rheumatic disease places on healthcare systems globally.
Artificial intelligence-assisted image analysis, digital biomarkers, and genomic profiling are beginning to influence early diagnosis and treatment stratification. These innovations carry the potential to identify patients at the highest risk of progressive erosive disease before irreversible damage occurs — a genuinely transformative prospect for the speciality.
For patients in the UAE seeking specialist input, the best hospitals in Qusais and surrounding districts have steadily expanded their rheumatology departments, offering access to biologic therapy, multidisciplinary care pathways, and advanced diagnostics that align with international clinical standards.
Why Rheumatology Deserves Greater Clinical Priority
Inflammatory arthritis, lupus, and related conditions collectively affect hundreds of millions of people worldwide, yet rheumatology workforce shortages remain a persistent challenge in both the UAE and the wider MENA region. Greater investment in training, early referral pathways, and public awareness campaigns carries enormous potential to reduce the long-term disease burden these conditions impose on patients, on healthcare systems, and on society at large. For clinicians across every speciality, a stronger working knowledge of rheumatology is not just academically worthwhile — it is clinically indispensable.
Write and Win: Participate in Creative writing Contest & International Essay Contest and win fabulous prizes.